http://shoulderarthritis.blogspot.mx/2014/02/revision-rate-survivorship-total.html
Saturday, February 8, 2014
Revision rate, survivorship, total shoulder
In outcome studies of shoulder arthroplasties we often use revision as the endpoint as a determination of ‘survivorship’. While there is no question that this endpoint is ‘objective’, the case below shows that the time to revision is actually subjective.
In 1996 the patient had a shoulder arthroplasty with a press fit stem and a cemented polyethylene glenoid component for rheumatoid arthritis. The initial films are no longer available.
Twelve years after surgery, at the age of 69 reporting that she had done very well with this for quite some time and was really having no difficulties with it until approximately 3-4 months prior to the visit. She wanted to begin working out at the Y and began experiencing increasing pain in her left shoulder. She stated that her pain was 5/10 and gradually worsening. She described it as sharp, exacerbated by activity. Rest and immobilization improved her pain. At that time her x-rays showed loose glenoid and humeral components
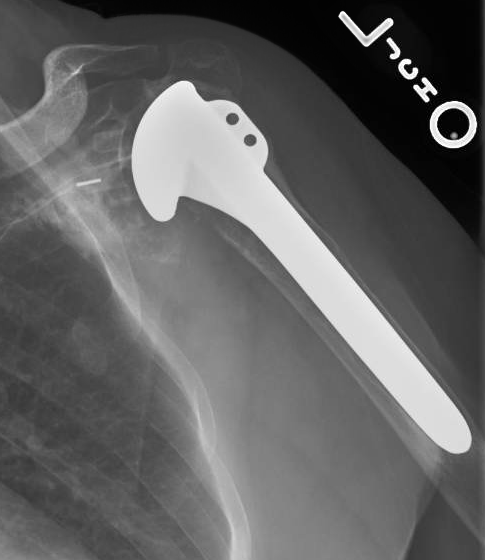
She did not wish a revision. Fourteen years after surgery she returned with ongoing discomfort and with these films.
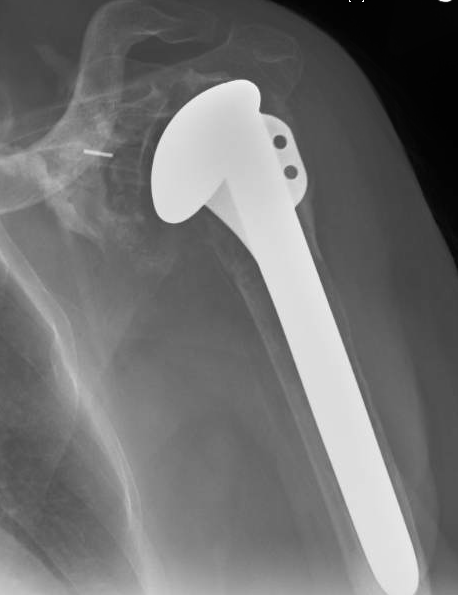
Same story at 16 years, note the medial migration of the glenoid component.
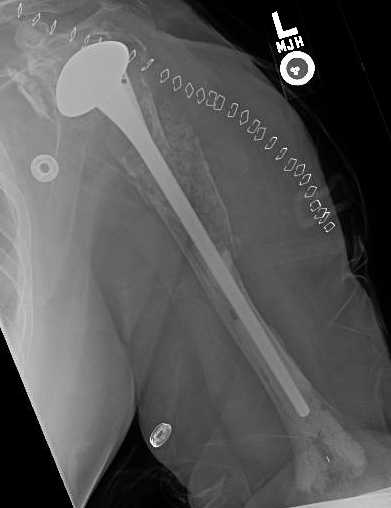
At 17 years she asked for a revision
At surgery she had severe osteolysis of the glenoid precluding replacement of a glenoid component and extremely fragile bone of the proximal half of the humerus. We used a long stem humeral prosthesis cemented in the distal third of the humerus and copious cancellous allograft proximally.
The point of this post is that her time to revision or the survivorship of the implant depended not on when the prosthesis failed (objective), but when the patient decided to have surgery (subjective). This emphasizes the point we’ve made in the past, the rate of failure is greater than the rate of revision.




Comentarios recientes